Do you have ongoing back pain? Here’s how GLA:D Back program at Nordica Health can help

Ongoing and/or recurrent back pain is very common—and it can be frustrating, confusing, and at times limiting. Many people find themselves trying different approaches and being told various things about what is causing their pain, leaving them unsure what is helpful, what to avoid, and how to move forward with confidence. Persistent pain or recurrent pain is pain that lasts longer than three to six months – including pain that comes and goes, even after tissues have healed. This means the approach to managing it is often different from a recent or acute injury (pain that has been present for less than three months). At Nordica Health, we are introducing the GLA:D Back program to support people in developing a clearer understanding of their back pain, and to build the confidence, skills, and capacity needed to manage their pain effectively. What is the GLA:D Back program? The GLA:D Back program is an evidence-based program originally developed in Denmark, designed for people living with persistent or recurrent low back pain. It includes: Education on most up-to date information about persistent and/or recurrent back pain Twice per week group exercise sessions with ongoing check-in and discussion Contribution to research on persistent and/or recurrent back pain What is the goal of the program? The aim of the program is to empower you to take an active role in your recovery and long-term management. This includes: Improving your understanding of back pain Building confidence in your body and movement Developing practical strategies to manage flare-ups Supporting long-term health and function The program also contributes to ongoing research, helping build the evidence base for future support and accessibility (including potential Medicare funding). https://vimeo.com/1192151245?share=copy&fl=sv&fe=ci What does the program include? Education sessions covering current, most-up to date evidence and understanding of persistent and recurrent low back pain Supervised group exercise sessions focused on improving strength, tolerance, and overall capacity The option to participate in a research database Individual assessments before and after the program to track progress Program structure at Nordica Health Our first GLA:D Back program will commence on 24th June, with limited places available. Schedule: Wednesdays: 2:30 – 3:30 pm Fridays: 1:30 – 2:30 pm Maximum of 5 participants per group Structure: Initial 1:1 intake and assessment (1 hour) Week 1: 2 x education sessions Weeks 2–9: 2 x exercise sessions per week (14 sessions total) Final 1:1 reassessment Interested in joining? Initial assessments will take place from late May through early June. If you would like to take part in the GLA:D Back program, please get in touch and we can arrange your initial assessment by emailing info@nordicahealth.com.au, or register your interest ->here<- to get contacted for more information.
Osteoporosis and Osteopenia
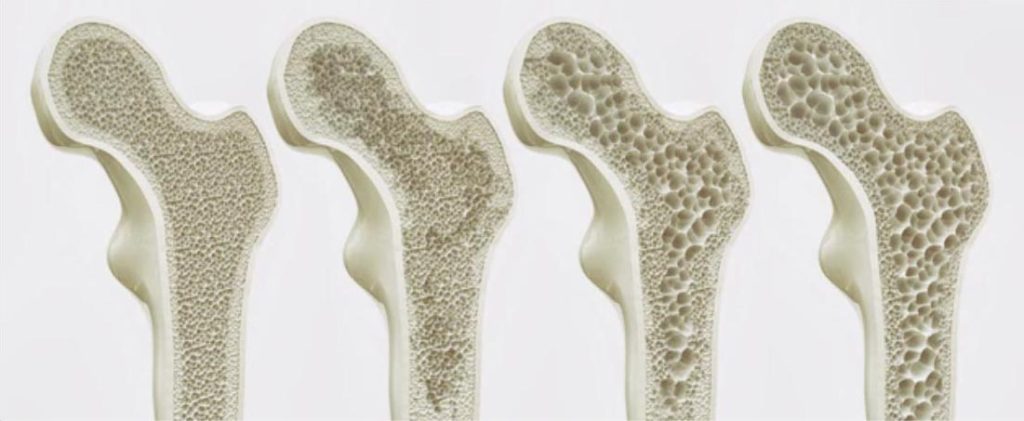
What is osteoporosis? Osteoporosis is a condition that weakens the bones and increases the risk of low traumatic fracture. The gold standard for diagnosing osteoporosis is the DXA scan, which measures Bone Mineral Density and provides a classification system to identify osteoporosis or osteopenia. Common body sites that are measured include the neck of femur, vertebrae of the lumbar spine, and occasionally the wrist. Low traumatic fractures are a significant risk worldwide, with 1 in 4 women and 1 in 5 men over 50 years old expected to sustain a fracture at some point in their lives. The impact of a fracture on an individual can result in fear avoidance of certain activities, loss of confidence, reduced mobility, strength, and functional capacity, a reduced quality of life, and depression or anxiety. How is osteoporosis assessed and diagnosed? Osteoporosis is a silent disease, and many people are unaware they have it until they sustain a fracture. If you have one or more risk factors, it is a good idea to discuss this with your GP and get a bone health assessment. Early diagnosis can help you take actions to improve your bone health, such as optimizing your diet, spending time in the sun, quitting smoking, reducing alcohol consumption, and commencing and maintaining a consistent osteogenic exercise routine. Osteoporosis can be diagnosed through three methods, which require confirmation that there is no other condition that appears to be osteoporosis but is not. The first method is a bone mineral density test that produces a T-score, with a score of -2.5 or below indicating osteoporosis. The second method is through a fracture, especially of the spine or hip, which suggests weak bones and the need for further evaluation. The third method involves using the FRAX fracture risk calculator, which assesses the chances of having different types of fractures in the next 10 years based on bone density, age, sex, height, weight, and answers to 7 questions. If the probability of a major osteoporotic fracture or hip fracture is above certain thresholds, a diagnosis of osteoporosis can be made. I have been diagnosed with osteoporosis, what do I do now? Exercise is one of the most effective non-pharmacological lifestyle changes that can influence bone strength and reduce the risk of fracture and falls, increase functional strength, improve confidence, reduce anxiety and depression, and improve overall quality of life. The Australian guidelines for physical activity recommend a minimum of 150 minutes per week of moderate-intensity aerobic exercise and at least two resistance training sessions per week to maintain a healthy life. However, exercise recommendations for osteoporosis focus on progressive resistance training, progressive impact training, and balance type activities. An Exercise Physiologist can help osteoporosis To optimize your bone health exercise plan, seek out an Accredited Exercise Physiologist or Physiotherapist who specializes in exercise for osteoporosis. At Nordica Health we complete a health screen and a thorough assessment will help tailor the exercise plan to your individual needs and preferences. Your starting point and maintenance phase will depend on your risk factors and individuality. Taking action to improve your bone health can reduce the risk of low traumatic fracture and improve your overall quality of life.
Osteoporosis awareness day

Step Up For Bone Health Today, Thursday the 20th of October is world osteoporosis awareness day, and we joined the campaign Step Up For Bone Health. Greta and I went to Cotton Tree Park to run our event “moving for healthy bones” to increase the awareness of what osteoporosis is, to identify risk factors, and to promote healthy lifestyle choices to improve bone health. Jessica interviewed on 109.4 (SunshineFM) for osteoporosis awareness day Exercise Physiologists Greta and Jessica talked about osteoporosis, and ran a movement session “Moving For Healthy Bones” on Osteoporosis Awareness Day. What is osteoporosis and osteopenia? Osteoporosis is a condition that weakens the bones, and increases the risk of low traumatic fracture. According to the World health organization, the gold standard to diagnose osteoporosis is through the DXA scan, which measures Bone Mineral Density, and provides a classification system to identify osteoporosis, or osteopenia. The common body sites that are measured are the neck of femur (hip) of non-dominant side, the vertabraes of the lumbar spine, and occasionally the wrist. Low traumatic fractures Worldwide; 1 in 4 women, and 1 in 5 men over 50 years old, will sustain a low traumatic fracture at some point in their life. Common fracture sites include; the vertebrae, the neck of the Femur (hips), wrists, ankles, toes, ribs. The impact of a fracture on somebody will depend on various factors, but can result in fear avoidance of certain activities, loss of confidence, reduced mobility, strength, and functional capacity; a reduced quality of life, depression and/or anxiety. Are you at risk? Risk factors for osteoporosis The majority of people who have osteoporosis will be unaware that they have it, until they sustain a fracture. This is why it is called a ‘silent disease’. If you have one or more risk factors, it might be a good idea to discuss this with your GP, and to get a bone health assessment. You can do so much more to increase your bone health by getting diagnosed early; before sustaining a fracture. Actions to improve your bone health includes: optimizing your diet (how, depend on your needs), spend 10-15 min in the sun per day, cease smoking, reduce alcohol consumption, and commence + maintain a consistent osteogenic exercise routine. Exercise prescription for osteoporosis: improve your bone health Exercise is one of the most effective non-pharmacological lifestyle change you can do that can not only substantially influence your bone strength, but can also reduce the risk of fracture and risk of falls, increase functional strength, improve your confidence, improve anxiety and depression, and improve your overall quality of life. The Australian guidelines of physical activity to maintain a healthy life include 1. Aerobic type exercise, a minimum of 150 min per week, at moderate exercise intensity, and 2. Resistance training, at least two times per week. However, if we are solely looking at exercise recommendations for osteoporosis, the guidelines are somewhat different. When implementing an exercise routine to assist in managing your osteopenia, osteoporosis, or preventing a reduction in bone strength, you can generally split them into three main categories. Progressive Resistance Training Progressive Impact Training Balance type activities Your starting point, and “maintenance point” (when you reach the maintenance phase), will be dependent on your risk factors, and your individuality. Get expert advise for your bone health exercise plan To optimize your bone health exercise plan, it would be a good idea to go through a health screen and assessment first. The exercise plan can then be tailored to suit your level of risk, preference and needs. We therefore recommend you seek out an Accredited Exercise Physiologist or Physiotherapist, who specializes in exercise for osteoporosis, before commencing an exercise plan to improve your bone health. Take the quiz Osteoporosis, and the risk of low traumatic fracture affects millions of people in the world, and you could be one of them. Take the quiz on worldosteoporosisday.org to identify any risk factors. If you are at risk, please discuss with your GP, and start implementing choices that your bones will thank you for. Get those bones moving; give them the specific exercise prescription they need.
Exercise protects our nervous system, and may prevent neurodegenerative diseases such as Alzheimer’s disease and Parkinson’s disease

Neurodegenerative diseases, such as Parkinson’s disease and Alzheimer’s disease, involves gradual deterioration of the structure and function of the nervous system. Progressive degeneration of the nervous system can be slowed down with the use of exercise. A recent study demonstrated a clear link between progressive resistance training and increased brain volume, and improved cognitive function after 12 months. https://www.abc.net.au/news/2020-02-11/strength-training-can-protect-brain-from-degeneration/11955646 There are a couple of theories to explain the results. When we exercise, many mechanical and physiological changes occurs, where a cocktail mix of molecules are being released into our blood stream. These molecules have many positive effects on our physical and mental health, and some molecules have neuroprotective properties that may induce neuroplasticity. Consistent and ongoing exercise also improve the electrical signals between nerv cells in the brain, making brain network more active and efficient. Nordica Health specialises in progressive resistance training for neurodegenerative diseases and osteoporosis on the Sunshine Coast, QLD Australia.
